Lessen Your Stress
Professor Judith Moskowitz developed a toolkit of eight skills, including practicing self-compassion and savoring positive events, that have been proven to reduce anxiety, boost your mood and improve well-being.
Physician-scientist Melissa Simon wants to make health care work for everyone. By Monika Wnuk
Melissa Simon will be the first to tell you that she wasn’t supposed to succeed.
“Where I grew up in Detroit, my family was in the bottom 1%,” says the vice chair for research in the department of obstetrics and gynecology at Northwestern’s Feinberg School of Medicine.
Seeing her own family members treated unfairly in health care settings gave Simon ’06 the resolve to become a doctor and change health care from the inside. As a physician-scientist, Simon is both a practicing doctor and a researcher. She combines research and community outreach to reduce gaps in health care services for medically underserved communities. Two of her main initiatives in this area center on preventing and treating cancer and decreasing maternal mortality among low-income women.
“It was important for me to be clinically active and take care of as many medically underserved women as I could, but I also needed to be a scientist so that I could make an impact on the population level,” she says. Simon founded the Center for Health Equity Transformation at Feinberg to serve as a research, education and training hub that promotes health equity and informs policy.
“Getting to health equality is not enough,” she says. “Equality assumes that resources should be distributed equally, but equity requires acknowledging that everyone needs a different type of lift.”
One track of Simon’s research seeks to improve access to preventive care and cancer treatment for low-income women.
“There are a lot of factors that can create barriers to access in public health care,” says Simon, “including proximity to resources, lack of information and the spread of misinformation.”
Over the last 15 years, Simon has studied these disparities and possible solutions — including patient navigator programs. Patient navigators are people local to a community who work with patients to address information and resource gaps, and connect them to health systems and community resources.
“In a nationwide study, we found that patient navigators can improve cancer outcomes for low-income and minority patients in both urban and suburban communities,” says Simon, “and we were then able to design more specific studies in Chicago and in the surrounding counties.”
In a 2019 study, Simon’s team went into Chicago’s Chinatown neighborhood to learn about the experiences of predominantly low-income women who had recently immigrated to the United States. The women who participated in these focus groups and interviews said that, because of language and transportation barriers, they would often only see doctors in the immediate Chinatown neighborhood and relied heavily on these doctors’ recommendations. The study found that many of these women were not getting mammograms because their doctors were not recommending them.
“The doctors weren’t prescribing mammograms because of a belief that Chinese women don’t get breast cancer, and we just know that’s a myth,” says Simon.
Next, Simon’s team hired patient navigators — health workers who lived in Chinatown and had the ability to bridge the trust between community members and the health care system. The navigators worked with community organizations and the local hospital to create a plan of care. As a result, more than 700 women from Chinatown participated in mammogram screenings, and those who had abnormal screening results were navigated through diagnostic screenings and initial treatment.
Opportunities to connect underserved communities to resources are one reason that Simon co-founded the Chicago Cancer Health Equity Collaborative (ChicagoCHEC), a team of researchers at the Robert H. Lurie Comprehensive Cancer Center of Northwestern University and two Chicago-area universities working in partnership with dozens of community organizations across the city.
Simon is also working to address another health care crisis among low-income women, one that hits especially close to her work as an obstetrician-gynecologist: maternal mortality.
“We’re the only industrialized country in the world where maternal mortality is rising,” says Simon. “That’s completely unacceptable.”
Specifically, Simon cites the 4-to-1 ratio between maternal mortality rates of African American and white women. To address this disparity in Chicago, Simon is working with the two largest networks of federally qualified health centers in Illinois to improve care in prenatal care clinics for African American women living on Chicago’s South and West Sides. Through a five-year grant, she will study the health care needs of pregnant African American women to develop a comprehensive perinatal care program. Simon and her team will evaluate that program in a clinical trial involving 600 women. To optimize perinatal care, this program will address social determinants of health — things like housing, food security, transportation and other factors.
“Our goal is to identify ways to improve everyday prenatal care for African American women, and most importantly, to tailor care to their needs,” says Simon. “Then, we want to use what we learn to scale that improvement in care for the entire country.”
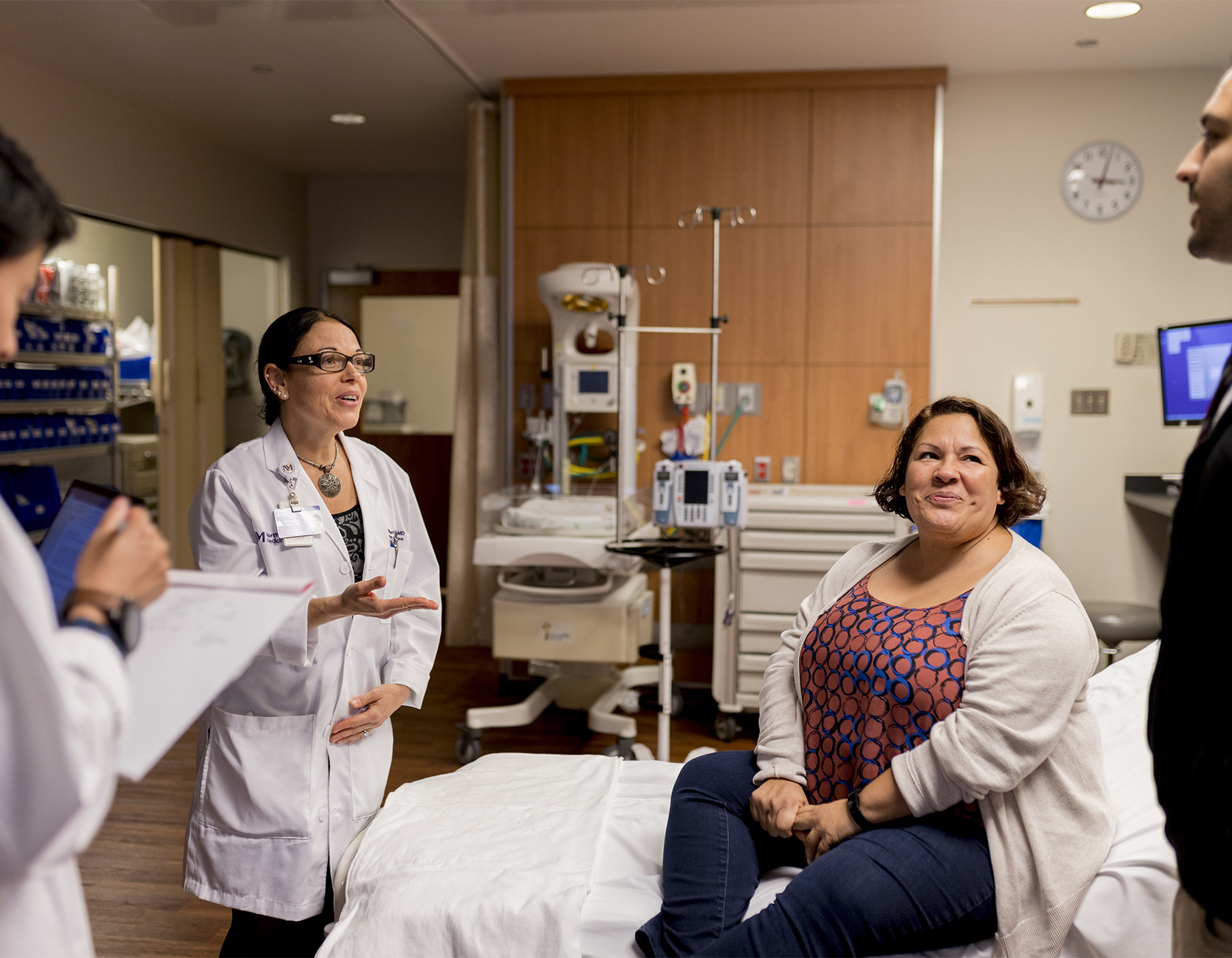
Simon admits that the road to creating the type of systemic change she’s after has never been easy, and that she didn’t always have role models in her personal or professional worlds to guide her.
“To be a trailblazer, you have to be brave because not many people at the top look like you,” she says. “Whether you succeed or fail, you will stand out. Staring failure in the face and accepting that it’s a necessary part of the path, that is what it takes to be trailblazer.”
To find that strength, Simon now turns to her network of female physician-scientists, including Pat Garcia ’91 GME, an OB-GYN and director of the Perinatal HIV Program at Northwestern Memorial Hospital. Garcia’s research has resulted in lower HIV transmission rates of the disease from mother to child.
“Pat Garcia’s research and policy work on perinatal HIV is a perfect example of what you can do as a physician-scientist and advocate,” says Simon. “Her passion for her work and her dedication to educating the next generation of physicians has been so inspirational to me and my own work.”
For her part, Garcia describes Simon as a “once-in-a-generation” leader.
“Her intellect and creativity as a scholar — as well as the passion for social justice that she applies to her work and also inspires in her students who will be the next generation to improve health outcomes in this country — demonstrates true leadership in this field,” says Garcia.
Mentoring future physicians is a high priority for Simon, and it’s the reason that research training and education is a part of most of her initiatives.
“My hope is that we continue to train students from diverse backgrounds to have both a nuanced understanding of health disparities,” says Simon, “and the drive to create and implement solutions across Chicago and around the world.”
Reader Responses
No one has commented on this page yet.
Submit a Response