Though Lindy Olive is only 29 years old, her lungs have been through a number of pulmonary challenges. As a newborn, she needed a special lung treatment to help her breathe. In 2019 she developed a deep cough and chest pain after being exposed daily to intense vinyl tile dust at her factory job in rural north Alabama. A month later, Olive was living and working next to an Environmental Protection Agency Superfund site (a contaminated area) and a landfill. Then, in 2021, she got sick with COVID-19.
“One day I was doing a high-intensity workout class, masked, and the next day, I could barely get up the stairs in my apartment without hinging at the waist to catch my breath,” recalls Olive, who moved to Chicago in 2019. “It was scary, and I wasn’t sure if I would fully recover.”
Luckily, Olive is now in good lung health. But those experiences left her wondering “how much my future lung health is going to be defined by what they have already been through.” So she enrolled in a national, first-of-its-kind millennial lung health study.
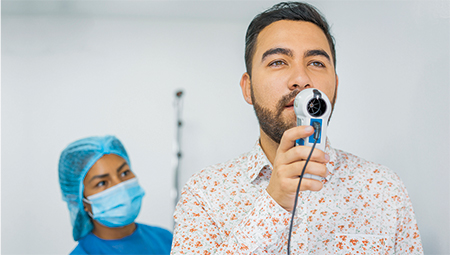
A patient uses a spirometer to test lung capacity. Credit: Getty Images/RicardoImagen
Launched by Northwestern University and the American Lung Association in May, the study will track and analyze lung health in millennials at the peak of their respiratory health. Scientists will follow 4,000 adults (ages 25 to 35) for about five years to evaluate how their environment and lifestyle affect respiratory health. Study participants are being recruited from 17 of the American Lung Association’s Airways Clinical Research Centers in metropolitan areas, including Chicago.
With lung disease now a leading cause of death in the country due to the increase in COVID-19 infections, the study is launching at an opportune time. Investigators have added COVID-19 exposures to their existing list of study measures, which include smoking, vaping, alcohol use, pollution and physical activity, providing an even fuller picture of millennial lung health than they originally imagined.
“The pandemic is probably one of the greatest exposures these participants will have on their overall health,” says principal investigator Ravi Kalhan ’07 MS, ’07 GME, professor of medicine and preventive medicine at Feinberg School of Medicine. “We are determined ... to better understand the short- and long-term impacts of COVID-19.”
With a $26 million grant from the National Institutes of Health’s National Heart, Lung and Blood Institute, Northwestern and other universities and hospitals will collaborate on the research. They hope to renew the grant so participants can be studied for the rest of their lives.
“What we know about our health and how to promote healthy aging is based on who we include in our research studies,” says principal investigator Mercedes Carnethon, professor of preventive medicine and medicine at Feinberg. “We are thrilled to [engage] young adults ... in our investigation.”
Olive, who earned a master’s degree in rural sociology and whose parents work in factories, sees benefits in understanding the long-term effects of environmental pollutants on local communities.
“The consequences of rural land use on health outcomes are understudied and ignored,” Olive says. “But being part of this study means researchers get to use my lung story to determine what makes the biggest impacts on lung health later in life.”
Read the press release in Northwestern Now for more.



Reader Responses
No one has commented on this page yet.
Submit a Response